Author’s note: The following passage is from the manuscript of my book, Summer in the Waiting Room: How Faith, Family, and Friends Saved My Life. This is the 47th excerpt in the series. Click on the image to read ALL excerpts.
*******************
The next morning, I had stabilized enough to move to the coronary care unit. The dilation issue with my eye was resolved and I started responding to commands and answering questions by shaking my head (I couldn’t talk with the tube blocking my vocal chords). Despite the fact that I was alert and responding, I don’t remember much in the hours and days following the cardiac arrest episode.
My sister Sisi arrived that morning. While she and Barbara were in the room with me, I used my limited sign language skills to communicate with them. Barbara learned to sign so she could converse with her oldest daughter, Becca, who is deaf. Sisi, close in age to Becca, learned at a young age and studied sign language formally. So, both of my sisters are fluent in American sign-language.
The first-born of my nieces and nephews, Becca stole my heart the minute I first saw her. I was just a kid and I mastered a few signs, which allowed me to talk with Becca in “broken” sign language. Barbara later recounted that I weakly signed to her and Sisi that I wasn’t going anywhere and to tell Sandra and the girls that I would be okay. Barbara interpreted my messages as a way to assure my family that I wasn’t giving up any time soon.
Later that day, Erica arrived from Washington, D.C. The flight home was uneventful with her friend Maya by her side. Other than small talk and junior high school girl gossip, they didn’t say much. Just as she had been after the heart attack twelve days before, Erica appeared as though the events of the past two weeks were nothing more than a bump in the road.
She later told me that faith kept her from worrying about what could happen and she believed that I would fight my way out of this. I have no memory of when she got to the room, but Sandra told me that I was alert and smiling when she walked in. Erica brought a couple of souvenirs for me, a copy of the Declaration of Independence and a baseball from the Smithsonian Institution. Sandra said I held the gifts in my hands like they were treasure.
Two days after the dreadful cardiac arrest, my lungs continued to clear and doctors considered removing the intubation tube. The plan moving forward once my lungs had stabilized was to consider options to resolve my heart issues. Unfortunately, as the effect of the sedatives weakened, I beat the doctors to the punch and removed the tube myself.
The tube inserted down my throat was almost a half inch in diameter and long enough to reach all the way to the trachea, which is the “windpipe” that goes directly into the lungs. I vaguely remember what it felt like to have the tube in my throat, and it’s a scary and helpless sensation. Pulling the tube out could have caused tremendous damage ripping through my windpipe, potentially scarring vocal chords and all tissue leading out of the mouth.
Once again, everyone was on high alert. When news reached the waiting room of my antics, Sandra uttered two words that would be repeated throughout the summer, “Now what?” Gathering around the doctor who had resolved the issue, everyone listened intently as he explained what had happened. According to a nurse, I was getting restless and tugging at the tube, and when the nurse turned away, I yanked it out.
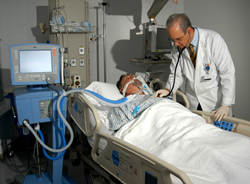
Scrambling quickly to stop any bleeding from the throat and continue providing oxygen to my lungs, doctors and nurses stabilized me and put a clear oxygen mask over my nose and mouth. To ensure that I didn’t pull the mask off, the nurse sedated me and strapped my hands to the bed to keep them from moving.
When Sandra finally saw me, I was fast asleep with a mischievous grin on my face and hands tied down. She couldn’t help chuckling with renewed hope because her travieso (troublemaker) was showing signs of life.
********************
Next Wednesday: Sandra and the girls inspire me to prepare for the fight of my life…








